Headache & Migraine
Migraine occurs with a throbbing pain that usually happens on one side of the head. The recurring headache of a migraine is triggered in situations of stress, hormonal imbalance and many more. In some cases, it may be accompanied by vomiting, nausea, pain in eyes or light sensitivity. Migraine attacks cause enormous pain in the head that may continue for hours or even days.
Migraines may or may not be accompanied by aura. What is Aura? Aura is linked to symptoms of the nervous system. These are the warning signs a person may experience before the migraine attack. The warning signals include blind spots, flashes of light, needle or tingling sensation in one arm or leg, feeling of numbness on the face or one side of body etc.
Looking onto the triggering factors of a Migraine
The cause of a migraine is not yet clear; however, it is linked to the unusual activities in the brain. The unusual changes in brain impact the normal working of the nervous system and lead to a chemical imbalance in the brain. The basic triggering factors of a migraine are as follows:-
Stress: Taking too much stress can trigger migraine condition in an individual. Other than stress, emotional triggers like anxiety, depression or shock can also cause severe pain.
Hormonal Imbalance: Changes in hormone can cause a migraine headache. Often, women during menstruation undergo changes in hormones that lead to a migraine.
Diet: Some food items are not good for migraine patients. These include citrus fruits, an excess amount of chocolates, cheese, caffeinated drinks, and alcohol. Adding to it, irregular eating patterns and not drinking enough amounts of water can be discomforting.
Physical Ailments: Not taking care of your lifestyle and body can cause a migraine to get severe. Improper sleep patterns, tiredness, pain in the shoulder area and a poor body posture can trigger the condition.
Medications: Intake of contraceptive pills, sleeping pills, or medications for hormonal replacement can be triggering.
Environmental Triggers: Some environmental conditions can also affect a headache. Loud music, flashing lights, strong smells, smoke can cause migraine pain. Some people may also feel discomfort in the crowd, bright lights or temperature changes.
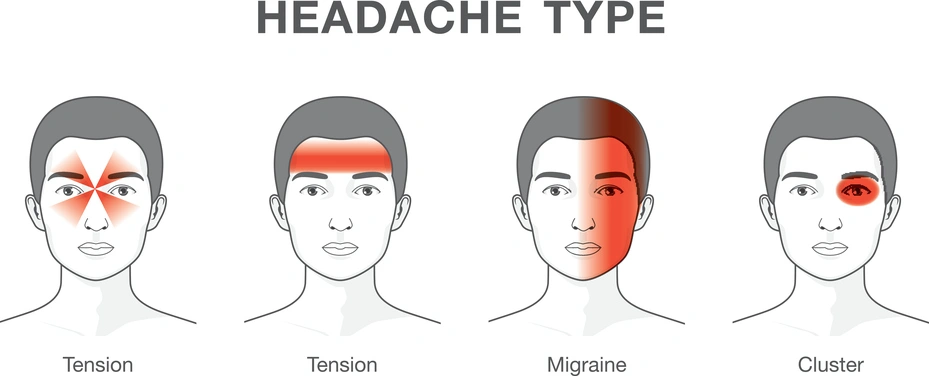
Cluster Headache: This is the most severe type of headache that causes a piercing pain behind or around an eye. It happens in clusters i.e., three times a day for 2-3 weeks in a month. The throbbing pain lasts for 15 mins to 3 hrs. It causes redness along with tears in the eye, drooping of the eyelids and the pupil to shrink. Also, the nostril on the affected side stuffs up.
Tension Headache: This is the most common type of headache that majorly affects adults and teenagers. The pain can be mild to moderate leading to the tightness of muscles. It causes pressure on the forehead, back of your head or neck. It is also known as a stress headache.
Thunderclap Headache: a Thunderclap headache is a very sudden and grows quickly. Causes may include a head injury or ruptured blood vessels. This can get serious if not consulted on time.
Occipital Neuralgia: This is a type of headache that is caused due to the injury of the occipital nerves. These nerves run from the top of the spinal cord to the scalp. It causes a throbbing pain much like an electric shock in the upper neck, back of the head and behind the ears. The pain usually happens on one side of the head.
Hemicrania Continua: Hemicrania Continua is a type of Chronic Daily Headaches. It causes a sharp stabbing pain on one side of the head. It can be chronic or remitting. It may happen three to five times a day. This type of headache is more common in women than men.
How can Migraine be treated?
Migraine is a result of several factors. And, there is no single treatment that can completely cure migraines. Most of the available treatments aim at eliminating the symptoms and saving the patient from instant migraine attacks.
Medication Treatment
For several people, medicines can work wonders to get rid of a migraine headache and attacks. The following medicines are usually prescribed to battle migraine pains:-
- Painkiller such as aspirin. The presence of ingredients; caffeine and acetaminophen reliefs severe headaches.
- Some over-the-counter medicines are; ibuprofen, naproxen, and acetaminophen.
- Metoclopramide is used to control the symptom of nausea and vomiting.
Nonconventional treatment
The surgical treatment for curing migraine includes botulinum toxin injections, which is injected into the nerves associated with migraines. These include the extracranial sensory branches of the trigeminal and cervical spinal nerves. This surgical procedure has proved to be effective in treating migraines.
Lifestyle Changes
Mild conditions of a migraine can be treated with certain lifestyle changes. These include:-
- Having enough sleep and following a good sleep pattern.
- Avoid taking the stress.
- Keep yourself hydrated.
- Gluten-free diet.
Stay active by including physical activities.
Common drugs used are responsible for autoregulation of blood vessels supplying the scalp and brain.
Vagus Nerve Stimulation
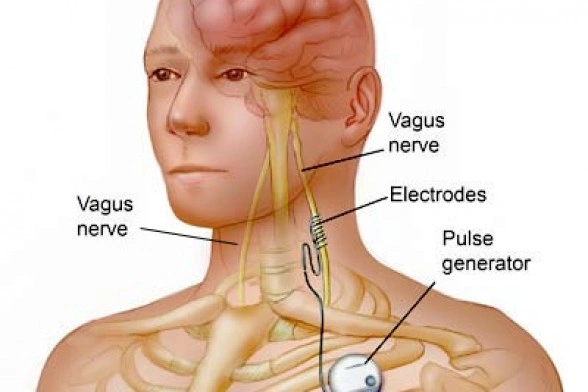
Vagus nerve stimulation is a USFDA approved device which is used to treat a Migraine, drug-resistant epilepsy or refractory epilepsy & Depression. VNS therapy or Device uses electrical impulses to stimulate the Vagus Nerve which is found on each side of the body from your brain through your neck to chest & Abdomen.
This consist of implanting a device under the skin in the left chest area. An electrode is attached with the generator device and placed under the skin. The wire is etched around the vagus nerve in the neck. A patient need not do anything with the device. The device will be programmed in the outpatient clinic to deliver the electric pulses or stimulation at regular intervals. The right vagus nerve is not used for the stimulation as it carries the fibers to the heart.
A person may not be aware of the stimulation. He can only be aware of when seizures happen. To send an extra burst of stimulation to the brain, the magnet can be swiped over the generator in the left chest.
Now, Noninvasive Vagus nerve stimulation devices are used which do not require surgical implantation and have been approved in Europe to treat head pain or a migraine, depression & epilepsy, It is approved by USFDA to treat headaches. Stimulation is done via Left Ear External Auditory Canal.
Migraine & COVID-19 FAQ
Question 1: Is Migraine a symptom of COVID-19? Answer: According to a report released by the World Health Organization (WHO), dose to 14% of people with COVI D-19 experience headaches. Headache is a broad term that may include Migraine headache before, it is possible that Migraine could be a symptom of COVID-19. However, other symptoms such as fever, dr cough & shortness of breath are more common in COVID-19 infection. A person should always look for these other signs of infection and contact the doctor if they experience these symptoms.
Question 2: Do people who suffer from Migraine are at a greater risk of COVID-19? Answer: Currently, there is no formal research looking at the relationship between Migraine and COVID-19 specifically. However, people who experience Migraine but are otherwise in good health are likely not at an elevated risk for COVID-19 or complications from COVID-19.
Question 3: Who are the people at more risk of COVID-19 infection?
Answer: Some groups of people are at more risk for severe complications from diseases such as C VID-19. At-risk individuals include those who:
Question 4: Is it afe to take NSAIDs to control in during Migraine attack i the time of COVID-19 pandemic? Answer: Non -steroidal anti-inflammatory drugs (NSAIDs) such as Ibuprofen, Diclofenac, Naproxen are the most commonly used as pain killer medicines. At present there is no sufficient scientific evidence connecting use of NSAIDs with worsening COVID-19 symptoms. Thus, you can use these medicines to control your pain during Migraine attack under the advice of your healthcare professional.
Question 5: I am very anxious and worried at this time of COVID-19 pandemic. Can stress trigger Migraine attack?
Answer: Stress can trigger Migraine for many people. COVI D-19 itself can be a source of stress, due to worrying about the infection or constantly hearing about it. Taking measures to reduce stress & anxiety during these times can help. Some tips to de-stress at home & reduce the chances of Migraines occurring:
Question 6: Does any Anti-Migraine medicine reduce immunity or pose increased risk of COVID-19 infection? Answer: There is no evidence that the medicines used in the treatment of Migraine suppress or activate the immune system or pose an increased risk of COVI -19 infection. Thus, if you get a Migraine attack, you should take the medicine as per your doctor's advice to control it.
Question 7: If I have Covid 19 infection, how can I manage migraine? Answer: People with COVID-19 who experience Migraine will still need treatment. People experiencing new headaches, including Migraine headaches, can try pain-relieving medicine such as Sumatriptan, Naproxen, Paracetamol, diclofenac etc. Drinking plenty of water and getting enough sleep, doing yoga, meditation may help reduce symptoms. Being Covid-19 positive, you need to observe physical distancing. Call your doctor, if you experience severe Migraine symptoms or your current medication does not control your attacks. The doctor can guide you through the teleconsultation i.e. virtual visits over mobile phones or computers. Be sure to have enough stock of your medicines.
Question 8: Are there any medicines to prevent Migraine attack? Should I take these medicines? Answer: Certain medicines such as Propranolol, Sodium Valproate, Topiramate are used to prevent Migraine attacks. If you suffer from Migraine attacks quiet frequently talk to your doctor who may prescribe preventive medications to you. However, do not use these medicines on your own without consulting your doctor. If you are already taking such preventive medications talk to your doctor about the continued use of these drugs. Be sure to have enough stock of your medicines.



